In the main article in this publication, the author points out various shortcomings of chronic pain management in the United States. In this commentary, I would like to address some of the reasons for such shortcomings as they pertain to the use of opioids for the management of chronic noncancer pain.
Chronic pain has been described as pain that has persisted for at least 1 month following the usual healing time of an acute injury, pain that occurs in association with a nonhealing lesion, or pain that recurs frequently over a period of months. In the majority of research and clinical reports, chronic pain is defined as pain that has persisted for at least 3 months.1,2 However, frustratingly few controlled trials on the use of opioids for noncancer chronic pain have had a duration longer than 6 weeks.3 Furthermore, no study of opioid therapy versus placebo, or opioid therapy versus nonopioid therapy, has evaluated pain, function, or quality of life for 1 year or longer.3 The few well-designed studies that have been conducted compared different long-acting opioids with each other,3 rather than comparing long-acting opioids with nonopioids or nonpharmacological treatment such as pain receptor blockage. In the absence of high-level evidence, stakeholders must rely on anecdotal evidence to determine treatment strategies.
Chronic pain is a very complex phenomenon, which may or may not be primarily driven by tissue injury. Traditionally, the most common forms of chronic pain have been divided into those labeled “nociceptive,” or pain caused by ongoing stimulation of pain receptors by tissue damage, and those labeled “neuropathic,” or pain that is most likely related to damage to, or dysfunction of, the peripheral or central nervous system. These categories of pain simplify a complex reality in which both acute and chronic pain are induced by multiple peripheral and central mechanisms, which continually interact with each other and with many pain-modulating systems. The perturbations that ultimately result in pain perception can be attributed to neurophysiologic processes and other related systems.4 For example, recent evidence is pointing to the role of neuroimmune activation following a tissue injury as an important mechanism in the development of chronic pain.5 The role of cytokines and other inflammatory mediators is obvious in inflammatory nociceptive pain, such as some types of arthritis, but animal data suggest an equally important role in the development of chronic neuropathic pain associated with central sensitization of neural pathways following peripheral injury.5
All chronic pain is profoundly influenced by psychological processing and responses.6 Pain severity and pain-related functional impairment are often found to be associated with psychological and social factors, and patients with identical diseases associated with pain, such as degenerative disk disease, may vary greatly in their reports of pain severity and pain behaviors.7 There is extensive literature documenting the importance of operant conditioning factors and cognitive-behavioral factors in the maintenance of chronic pain behaviors.8
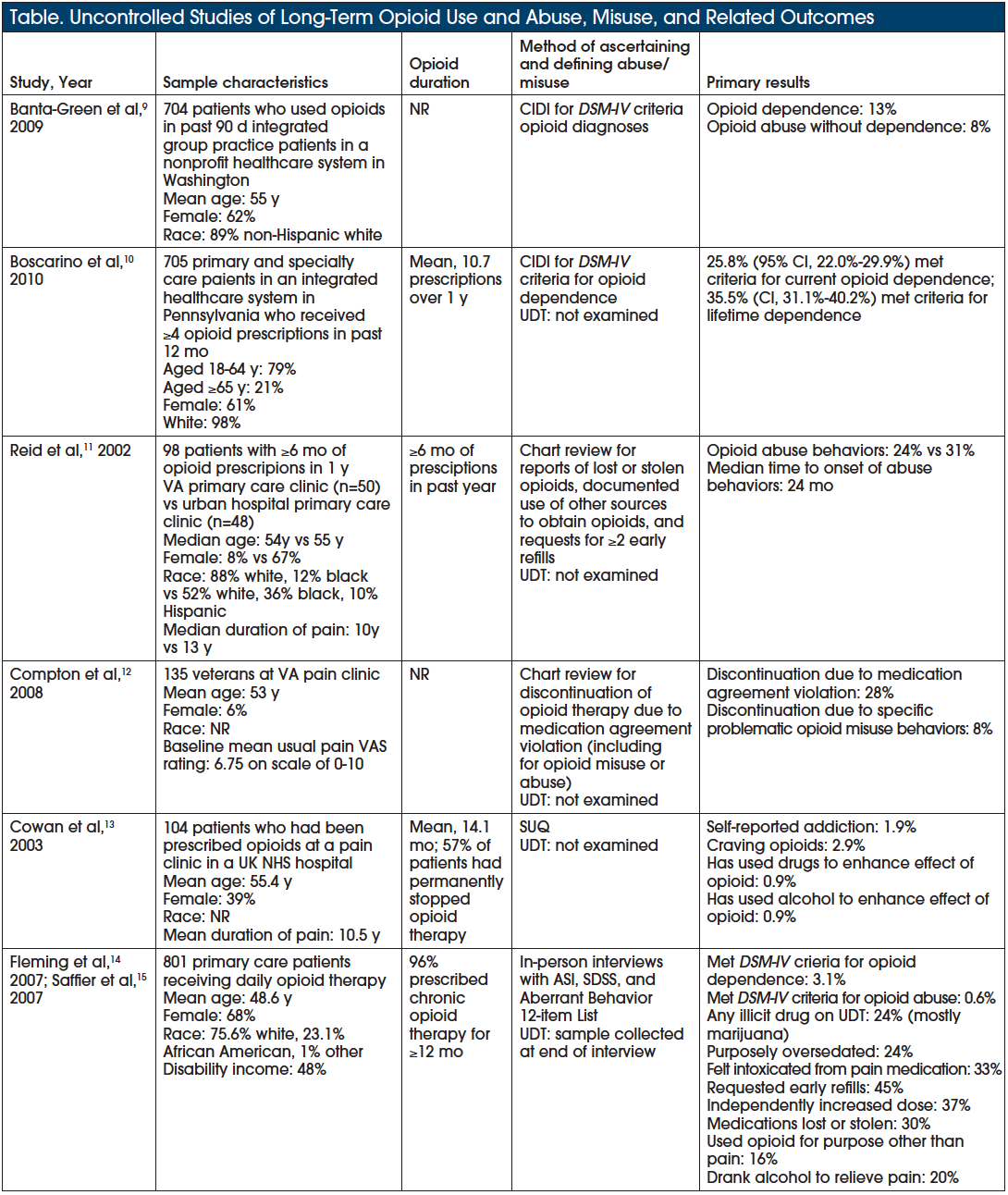
In contrast to the lack of clarity about whether opioids are useful for pain management, an abundance of data point to their harmful effects.3 These include increased risks for fracture, addiction, sexual dysfunction, cardiovascular events, endocrinologic harms, and traffic accidents.3 There is also substantial evidence from uncontrolled studies regarding the problems of opioid dependence and misuse (Table).3,9-19
We will continue to see gaps in chronic pain management until better therapeutic options become available, including, but not limited to, novel, nonopioid medications.

References
- Verhaak PF, Kerssens JJ, Dekker J, et al. Prevalence of chronic benign pain disorder among adults: a review of the literature. Pain. 1998;77:231-239.
- Franklin GM. Opioids for chronic noncancer pain: a position paper of the American Academy of Neurology. Neurology. 2014;83:1277-1284.
- Chou R, Turner JA, Devine EB, et al. The effectiveness and risks of long-term opioid therapy for chronic pain: a systematic review for a National Institutes of Health Pathways to Prevention Workshop. Ann Intern Med. 2015;162:276-286.
- Rosenblum A, Marsch LA, Joseph H, et al. Opioids and the treatment of chronic pain: controversies, current status, and future directions. Exp Clin Psychopharmacol. 2008;16:405-416.
- DeLeo JA. Basic science of pain. J Bone Joint Surg Am. 2006;88(suppl 2):58-62.
- Turk DC, Melzack R. The measurement of pain and assessment of people experiencing pain. In: Turk DC, Melzack R, eds. Handbook of Pain Assessment. 2nd ed. New York, NY: Guilford Press; 2001:3-14.
- Aronoff GM, ed. Evaluation and Treatment of Chronic Pain. New York, NY: Lippincott, Williams & Wilkins; 1999.
- Fordyce WE. Behavioural Methods for Chronic Pain and Illness. St. Louis, MO: CV Mosby; 1976.
- Banta-Green CJ, Merrill JO, Doyle SR, et al. Measurement of opioid problems among chronic pain patients in a general medical population. Drug Alcohol Depend. 2009;104:43-49.
- Boscarino JA, Rukstalis M, Hoffman SN, et al. Risk factors for drug dependence among out-patients on opioid therapy in a large US health-care system. Addiction. 2010;105:1776-1782.
- Reid MC, Engles-Horton LL, Weber MB, et al. Use of opioid medications for chronic noncancer pain syndromes in primary care. J Gen Intern Med. 2002;17:173-179.
- Compton PA, Wu SM, Schieffer B, et al. Introduction of a self-report version of the Prescription Drug Use Questionnaire and relationship to medication agreement noncompliance. J Pain Symptom Manage. 2008;36:383-395.
- Cowan DT, Wilson-Barnett J, Griffiths P, et al. A survey of chronic noncancer pain patients prescribed opioid analgesics. Pain Med. 2003;4:340-351.
- Fleming MF, Balousek SL, Klessig CL, et al. Substance use disorders in a primary care sample receiving daily opioid therapy. J Pain. 2007;8:573-582.
- Saffier K, Colombo C, Brown D, et al. Addiction Severity Index in a chronic pain sample receiving opioid therapy. J Subst Abuse Treat. 2007;33:303-311.
- Højsted J, Nielsen PR, Guldstrand SK, et al. Classification and identification of opioid addiction in chronic pain patients. Eur J Pain. 2010;14:1014-1020.
- Portenoy RK, Farrar JT, Backonja MM, et al. Long-term use of controlled-release oxycodone for noncancer pain: results of a 3-year registry study. Clin J Pain. 2007;23:287-299.
- Schneider JP, Kirsh KL. Defining clinical issues around tolerance, hyperalgesia, and addiction: a quantitative and qualitative outcome study of long-term opioid dosing in a chronic pain practice. J Opioid Manag. 2010;6:385-395.
- Wasan AD, Butler SF, Budman SH, et al. Does report of craving opioid medication predict aberrant drug behavior among chronic pain patients? Clin J Pain. 2009;25:193-198.
